Chronic stress does not simply mean “too much cortisol”. Rather, it alters how the stress system functions over time. This can involve prolonged responses, reduced feedback sensitivity, disrupted daily rhythms and, in some cases, blunted responses.
These patterns vary between individuals and can show up in different ways, including:
- Prolonged responses to stress
- Reduced sensitivity to feedback signals
- Altered daily rhythms
- Blunted or reduced responses
Your body becomes less responsive
With continued stress, your body becomes less sensitive to cortisol’s signals. This is sometimes referred to as reduced glucocorticoid sensitivity. When this happens, the feedback system that normally switches off the stress response becomes less effective, meaning the body finds it harder to return to balance.
Inflammation can increase
Cortisol normally helps regulate inflammation. In the short term, it can reduce inflammatory activity.
However, with chronic stress, the immune system can become less responsive to cortisol. This has been associated with a gradual increase in low-level inflammation, which has been linked to some forms of depression, although this relationship is not consistent across all individuals.
Changes in brain chemistry
Chronic stress has been associated with changes in how the body processes tryptophan, an amino acid used to produce serotonin.
Under prolonged stress, more tryptophan may be diverted into the kynurenine pathway rather than being used to make serotonin. This may influence the availability of serotonin, although this varies across individuals and contexts.
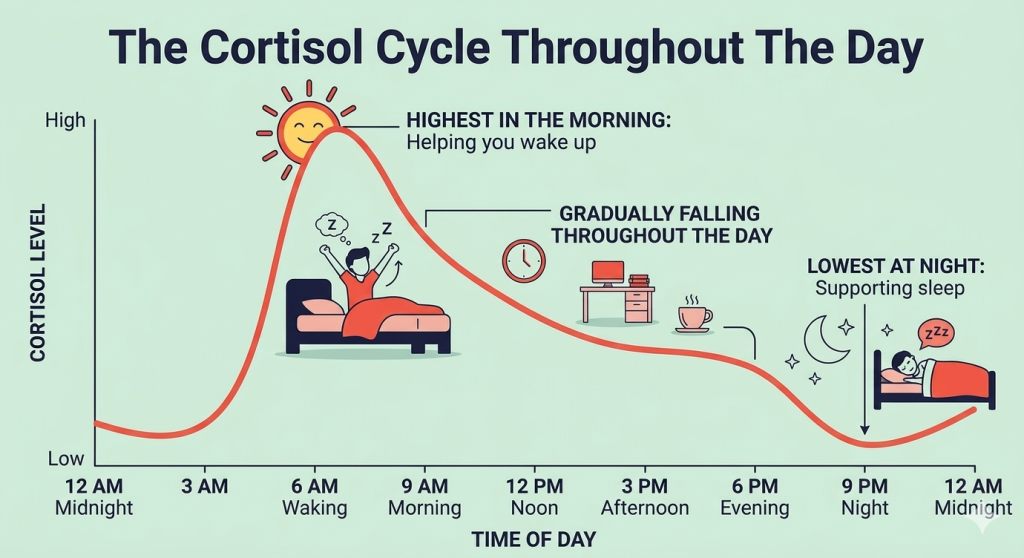
Your body clock can shift
Stress often affects sleep and daily routines. Over time, this can disrupt your internal body clock, leading to:
- Difficulty falling or staying asleep
- Lower energy during the day
- Further disruption to stress hormones
These effects can reinforce each other, creating a cycle that is hard to break.